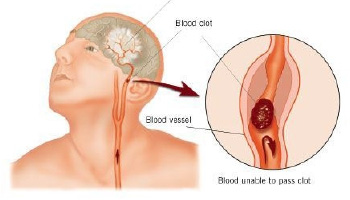
The July issue of the Journal of the American Medical Association has just published new data showing that the rate of stroke, the 4th leading cause of death in the US, has dropped steadily over the last 20 years. A fantastic result validating 2 decades of advancing medical practice!
What reduced the risk of stroke and death from stroke?
Researchers attribute the dramatic results to successful treatment of risk factors such as high cholesterol and hypertension, and a reduction in the number of people who smoke tobacco. The magnitude of benefit was greatest in adults over age 65, where the use of cholesterol lowering medication and blood pressure medication has increased the most. Effects were more modest for middle aged adults, and researchers point out that rising rates of obesity and diabetes in the middle aged population might reverse this trend as we see more obesity in elderly adults.
How big was the effect?
The rate of death from stroke dropped 25% and the number of strokes fell by 20%.
What is my risk of stroke?
A variety of tools have been published allowing patients and physicians to estimate an individual person’s risk of stroke and heart attack. Most of them predict 10 year risk, so the calculators apply best to patients over age 50 where the risk of stroke and heart attack is easier to measure and benefits are more obvious. Click here for one example of a Risk Estimation Calculator.
Putting a variety of hypothetical numbers into the calculator can be a very informative demonstration of the power of controlling blood pressure, treating high cholesterol, or quitting smoking.
Does treating my risk factors before age 50 make a difference?
Even though the risk calculators won’t show such impressive changes when applied to younger patients, we know that early and aggressive treatment of smoking, obesity, hypertension and high cholesterol have a huge impact on health later in life.
The MyLifeCheck campaign from the American Heart and American Stroke association presents what we know about heart attack and stroke risk reduction in younger patients very clearly. Visit their excellent website to learn more.
What can I do now?
The answer is obvious but not necessarily easy: eat well, exercise, and don’t smoke. If you have questions about healthy lifestyle choices, if you need help quitting smoking, or if you are interested in finding out more about your blood pressure and cholesterol numbers, check in with your physician. We would be glad to help!